Nearly half of American adults over 30 have some form of periodontal disease, according to data from the Centers for Disease Control and Prevention. That number climbs to roughly 70 percent among adults over 65. The reason it does not feel that way is straightforward: gum disease usually does not hurt, at least not in its early stages, and pain is what most people use as the trigger for seeing a dentist. At All Smiles Dental in Burley, Dr. Spencer Rice regularly sees patients who have been walking around with significant gum disease for years, often patients who describe their teeth as fine because nothing was bothering them. That disconnect between what patients feel and what is actually happening in their mouths is the defining challenge of periodontal health.
Gingivitis vs. Periodontitis: The Difference That Determines Your Options
Gum disease is not a single condition. It exists on a spectrum, and where a patient falls on that spectrum determines both the urgency of treatment and what treatment looks like.
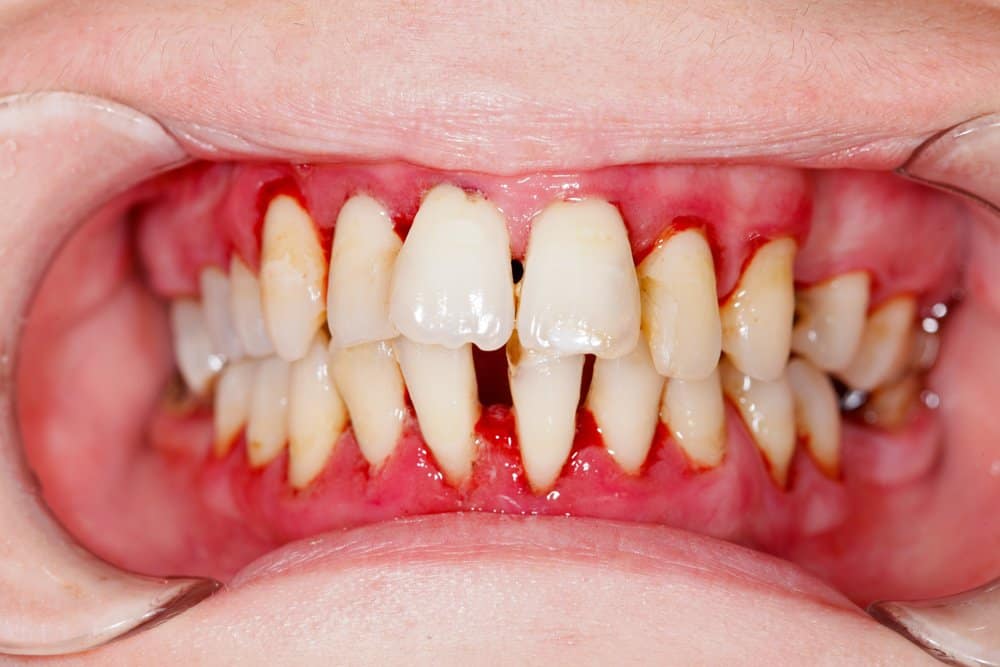
Gingivitis is the earliest stage. It is inflammation of the gum tissue caused by the accumulation of bacterial plaque along and just beneath the gumline. The gums may look slightly red or swollen, bleed when brushed or flossed, and feel tender in some cases. In others, there are no noticeable symptoms at all. Critically, gingivitis is reversible. The bone and connective tissue supporting the teeth have not yet been damaged. A professional cleaning to remove the calculus that has built up, combined with improved home care, can resolve gingivitis entirely. No tissue has been lost that cannot be recovered.
Periodontitis is what gingivitis becomes when it is left untreated long enough. The bacterial infection moves below the gumline and begins to destroy the bone and periodontal ligament that anchor the teeth in the jaw. As that bone is lost, the gum tissue pulls away from the tooth, creating periodontal pockets where bacteria accumulate and cause further destruction. This damage is permanent. Bone lost to periodontitis does not grow back on its own, and the teeth that depend on that bone for support become progressively looser over time.
The transition from gingivitis to periodontitis is not dramatic or sudden. It happens gradually, over months and years, with no pain signal alerting the patient that anything significant is happening. Many patients first learn they have periodontitis when they begin to notice tooth mobility or when they finally see a dentist after a long gap and the x-rays reveal bone loss that has been accumulating quietly.
The Systemic Connection: Why Gum Disease Is Not Just a Dental Problem
For a long time, periodontal disease was viewed almost exclusively as an oral health issue. That view has shifted substantially over the past two decades as research has established consistent associations between gum disease and several serious systemic health conditions.
The connection to cardiovascular disease is the most studied. People with periodontitis have a significantly higher risk of heart disease, heart attack, and stroke than people with healthy gums. The leading explanation is that the chronic bacterial infection in the gums allows inflammatory mediators and even bacteria themselves to enter the bloodstream, where they contribute to the inflammation that drives atherosclerosis. The oral bacteria Porphyromonas gingivalis, one of the primary pathogens in periodontitis, has been found in arterial plaques, a finding that has changed how cardiologists think about oral health.
The relationship between gum disease and diabetes runs in both directions. People with poorly controlled type 2 diabetes are significantly more susceptible to periodontal disease because elevated blood sugar impairs immune function and creates an environment where oral bacteria thrive. At the same time, the chronic inflammation from periodontitis makes blood glucose harder to control, worsening diabetic outcomes. Treating gum disease in diabetic patients has been shown in multiple studies to produce measurable improvements in HbA1c levels, the standard long-term marker of blood sugar control.
Associations have also been documented between periodontal disease and adverse pregnancy outcomes, including preterm birth and low birth weight, as well as with respiratory conditions including chronic obstructive pulmonary disease and pneumonia. The common thread across all of these connections is chronic systemic inflammation, and the mouth is a significant and often ignored contributor to that inflammatory burden.
Why Idaho Adults Are Particularly at Risk
Idaho’s rates of smoking and tobacco use are above the national average in many rural counties, and tobacco is one of the strongest risk factors for periodontal disease. Smoking impairs circulation in the gum tissue, reduces the mouth’s immune response to bacteria, and masks the bleeding and redness that are the most visible early signs of gingivitis. Smokers are significantly more likely to develop periodontitis and significantly less likely to respond well to treatment compared to non-smokers.
Idaho also has meaningful rates of diabetes and obesity, both of which independently elevate periodontal risk. And like many rural communities, access to regular dental care in parts of the Magic Valley is limited enough that gaps between dental visits stretch into years for many adults, which allows early gum disease to progress well past the reversible stage before anyone catches it.
Dry mouth, which affects a significant proportion of adults taking multiple medications, is another contributor. Saliva is the mouth’s natural defense mechanism against bacterial accumulation, and a chronically dry oral environment accelerates both tooth decay and gum disease. Adults who take medications for blood pressure, allergies, depression, or bladder conditions are commonly affected and often do not realize it.
What Modern Gum Disease Treatment Actually Involves
The treatment for gum disease depends entirely on how far the disease has progressed. For patients with gingivitis, a thorough professional cleaning to remove plaque and calculus, combined with instruction on effective home care technique, is often all that is needed. Many patients in this category see their gum health return to normal within a few weeks if they follow through consistently.
Periodontitis requires a more involved procedure called scaling and root planing, sometimes referred to as a deep cleaning. Where a standard cleaning addresses the tooth surface above and just at the gumline, scaling and root planing extends below the gumline into the periodontal pockets to remove calculus and bacterial deposits from the root surfaces. The root surfaces are then smoothed, which makes it harder for bacteria to reattach and helps the gum tissue reattach to the tooth at a healthier level. The procedure is typically done in quadrants under local anesthesia over one or two appointments.
After active periodontal treatment, patients move into a maintenance phase with more frequent hygiene appointments, typically every three to four months rather than the standard six-month interval. This schedule exists because the bacteria responsible for periodontitis recolonize below the gumline within about 90 days without intervention. Periodontal maintenance is not optional for patients who have had active disease. It is what keeps the condition stable rather than progressing.
What Patients Who Have Avoided the Dentist for Years Can Expect
One of the most common things Dr. Rice hears from patients who have been away from dental care for a long time is that they are embarrassed about the state of their teeth and are not sure what kind of reaction to expect when they come in. At All Smiles Dental, the response is practical, not judgmental. The goal of the first appointment is to find out where things actually stand so that a realistic treatment plan can be built, not to make a patient feel worse about a gap in care they may have had very understandable reasons for.
Periodontal disease that has progressed significantly over years of deferred care cannot be resolved in a single visit, and any dentist who suggests otherwise is not being honest. But it can almost always be arrested and stabilized with a proper course of treatment and a commitment to maintenance afterward. Patients who have lost teeth to periodontitis may eventually want to discuss replacement options like dental implants. But the starting point is always the gum disease itself, because implants placed in a mouth with uncontrolled periodontal disease will fail for the same reasons the natural teeth did.
Getting Back on Track at All Smiles Dental in Burley
Gum disease is both common and treatable. The two things that work against patients are waiting until something hurts and assuming that a long gap in dental care means the situation is beyond help. Neither is true. Early-stage disease is reversible. More advanced disease is manageable. And the health consequences of leaving periodontitis untreated, for the teeth and for the rest of the body, are significant enough that getting evaluated is genuinely worth prioritizing.
All Smiles Dental serves patients throughout Burley, Twin Falls, and the wider Magic Valley area in a practice specifically designed to make dental care approachable for people who have had anxiety about coming in. If you have been avoiding the dentist, if your gums bleed when you brush, or if it has simply been longer than you would like to admit since your last cleaning, a call to Dr. Rice’s office is the right first move. The conversation about where you are and what to do about it starts there.